There are no products in your shopping cart.
| 0 Items | £0.00 |
If you have questions or need to talk, call our helpline for information or support.
Have a question? Receive a confidential response via email.
Come to a support event to meet other people who have had a cervical cancer diagnosis.
Connect with others, share experiences and ask questions on our forum.
Individual support via phone or email, for anyone affected by a cervical cancer diagnosis.
Read about ways to cope with any effects of treatment and getting practical support.
June 2023 — Please be aware that this page is currently undergoing review. However, the information
stated is valid.
At your cervical screening (smear test) appointment, a nurse takes a sample of cells from your cervix using a small, soft brush. The test only takes a few minutes.
If you feel worried about going for cervical screening, you are not alone. It may help to know as much as possible about what going for cervical screening is like. You could ask someone you trust about their experience, speak with your nurse or doctor, or call our free Helpline on 0808 802 8000 for more support.
If you are registered with a GP, you will get a letter telling you it is time for your cervical screening appointment. You have to contact your GP to book an appointment. You can usually do this online or over the phone.
In some areas, sexual health clinics offer cervical screening. You may choose to contact your local clinic if you aren’t able to access, or don’t feel comfortable at, your GP surgery.
Read our blog about what to expect at your cervical screening appointment >
Many GP surgeries offer cervical screening appointments on set days or at set times. If you can’t attend any of the available appointments, speak to your GP surgery to see if they can be flexible for you.
Plan to spend at least 30 minutes at your GP surgery, which may include waiting for your appointment or being directed to the room. The test itself, where your nurse takes a sample of cells from your cervix, will only take a few minutes.
Your GP surgery will give you details about what to do once you arrive.
Although face coverings are no longer mandatory in healthcare settings, you can still choose to wear one if you wish
A nurse, sometimes called a sample taker, will invite you into a treatment room. They will explain what cervical screening is and check if you have any questions.
Your GP surgery will follow local guidance about wearing PPE. If your nurse is wearing PPE, this may include a mask, gloves and apron.
Your nurse will give you a private space to undress from the waist down, usually behind a curtain. If you are wearing a dress or skirt, you can leave this on and just take off your underwear.
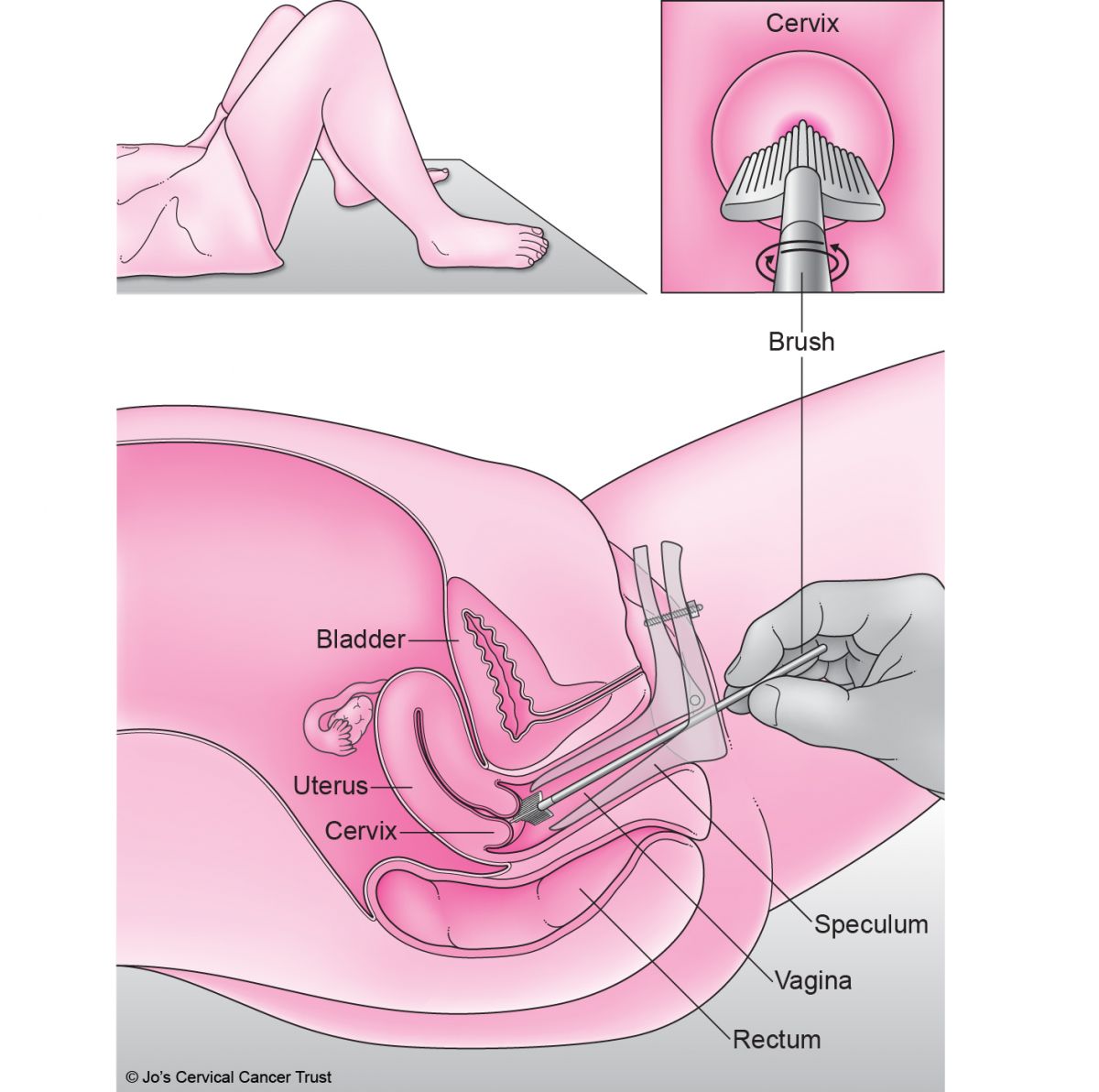 Your nurse will ask you to lie on an examination bed and give you a new, clean paper sheet to cover the lower half of your body. You can lie:
Your nurse will ask you to lie on an examination bed and give you a new, clean paper sheet to cover the lower half of your body. You can lie:
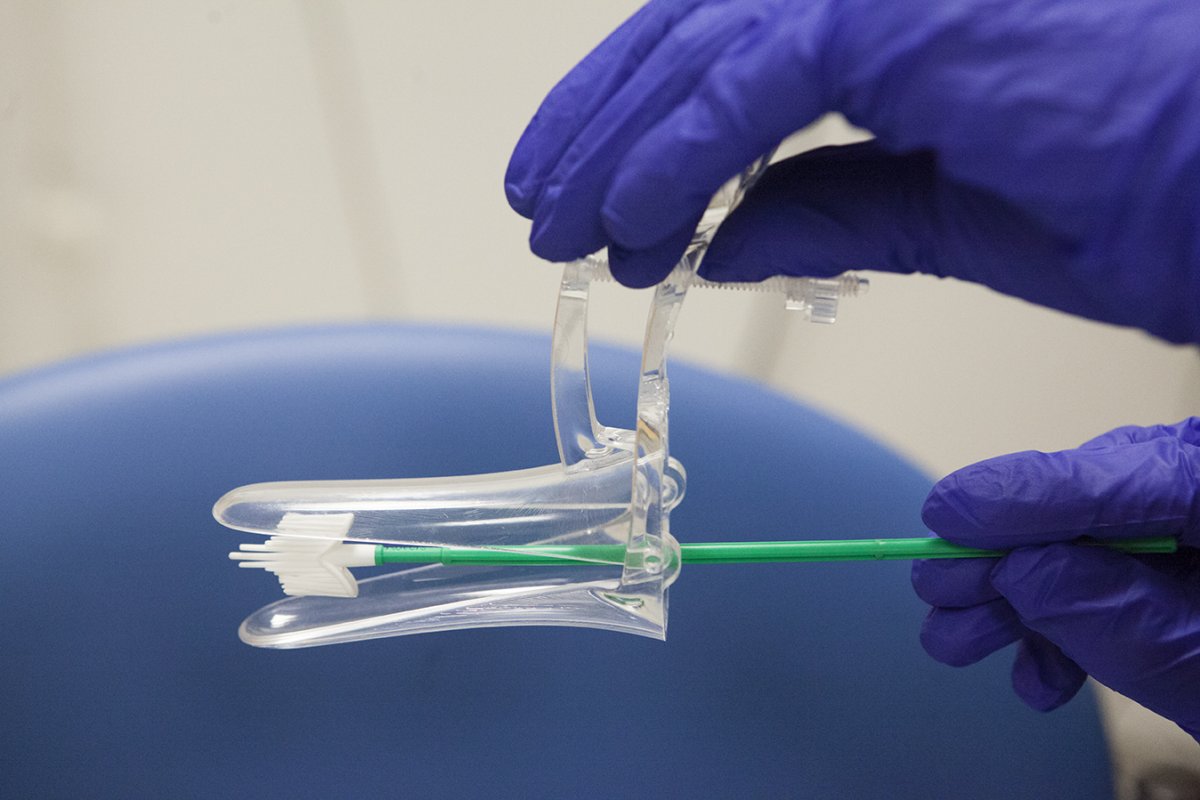
Your nurse will let you know when the test is about to start. First, they gently put a new, clean speculum into your vagina. A speculum is usually a plastic cylinder with a round end – sometimes a metal speculum is used. The speculum is the part that some people find uncomfortable.
Once the speculum is inside your vagina, the nurse will gently open it so they can see your cervix.
Then the nurse will use a small, soft brush to quickly take a sample of cells from your cervix. This may feel a bit strange, but should not be painful.
The nurse will put your sample of cells into a small plastic container (vial) of liquid. The liquid preserves the cells so they can be sent to a lab for testing.
And that’s it! The nurse will take the speculum out of your vagina and give you a private space to dress again. They will explain how and when you should get your results.
Read about how your sample is tested >
Most people can continue their day as usual after the appointment.
You may have some light bleeding (spotting) for a day after the test, so it can help to wear a sanitary pad or panty-liner.
Your cervical screening results should arrive by post within 4 weeks.
Read about cervical screening results >
Everyone’s experience of cervical screening is different. Some people don't find it uncomfortable, while for others it may be uncomfortable or hurt. There are lots of reasons, physical and pyschological, for this. It is important to tell your nurse or doctor if cervical screening is painful for you.
If you want to go for cervical screening, there are ways to make the test more comfortable and make sure you get the right support.
No. Jo's Cervical Cancer Trust is a charity independent of the national cervical screening programme, GP surgeries and other clinics and cannot book a cervical screening appointment for you.
If you want to book a cervical screening appointment, contact your local GP. Some sexual health services in your area may also offer cervical screening.
Read about how coronavirus has affected booking a cervical screening appointment >
Whether it’s your first time or you have been before, we know that going for cervical screening may make you feel anxious. It may help to remember that everyone has a different experience of cervical screening. If you need any support, it is important to let your nurse or doctor know.
Read our blog on deciding whether to go for cervical screening >
We have more information about:
If you have questions or need some emotional support, our Helpline is open on 0808 802 8000.
Check our Helpline opening hours >
We also have a welcoming community in our online Forum, where you can get and give support. There are lots of conversations about cervical screening, so you can choose to read existing threads or post your own messages.
Thank you to all the experts who checked the accuracy of this information, and the volunteers who shared their personal experience to help us develop it.
We write our information based on literature searches and expert review. For more information about the references we used, please contact [email protected]

Help us keep our vital support services running by donating £20 to fund a call to our Helpline.
Find out how cervical screening samples are tested.

Talk to someone about how you’re feeling, or connect with others on our Forum.

